Description of transurethral resection for a bladder tumour (TURBT
TURBT is a primary treatment for all types of bladder cancer. If the cancer is limited to the superficial layer of the bladder, it may be the only treatment needed. It’s a one-day surgery, and the anesthesia used can be either general or spinal.

How is a bladder tumour resection performed?
Dr. Marois performs surgeries that require an anesthesiologist at the Montreal Centre Métropolitain de Chirurgie, which is the only accredited private hospital in Quebec. He uses the latest methods and technology: bipolar transurethral resection in saline (which further limits complications) and a high-resolution camera.
Dr. Marois begins by inserting a cystoscope (a thin, rigid tube with a light and a lens) into the urethra and sliding it into the bladder. He then inserts a bipolar plasmaloop rectoscope into the cystoscope to remove the tumour and a small amount of the surrounding normal tissue.
During a TURBT operation, he will also remove tissue from the bladder wall. This sample will be analyzed to see if the cancer has infiltrated the layer of muscle in the bladder wall. Dr. Marois will then cauterize the area where the tumour was removed using a high-
energy electric current (fulguration). This procedure will seal the blood vessels and destroy any remaining cancer.
What can you expect following a TURBT procedure?
● You’ll remain in recovery for a few hours after the surgery so that the hospital’s nursing staff can keep an eye on you.
● Using a catheter, the inside of your bladder will be cleaned periodically with a watery solution to flush out traces of blood (a normal procedure after this type of surgery).
● The catheter may cause discomfort or spasms in the bladder. If this is the case, medication can be administered to provide relief. You’ll also have a daytime thigh bag and an overnight drainage bag.
● You’ll return home the same day, but you’ll need to be accompanied by someone.
● The catheter will be removed after five days; this can be done either at a CLSC near your home or at Dr. Marois’ office.
● Once the catheter has been removed and you are able to urinate naturally, you may feel an increased urgency or even some pain when urinating. This tends to disappear as inflammation goes down and the muscles strengthen.
● Using a catheter, the inside of your bladder will be cleaned periodically with a watery solution to flush out traces of blood (a normal procedure after this type of surgery).
● The catheter may cause discomfort or spasms in the bladder. If this is the case, medication can be administered to provide relief. You’ll also have a daytime thigh bag and an overnight drainage bag.
● You’ll return home the same day, but you’ll need to be accompanied by someone.
● The catheter will be removed after five days; this can be done either at a CLSC near your home or at Dr. Marois’ office.
● Once the catheter has been removed and you are able to urinate naturally, you may feel an increased urgency or even some pain when urinating. This tends to disappear as inflammation goes down and the muscles strengthen.
What risks and complications are associated with TURBT?
In the majority of bladder tumour removal cases, there are few to no complications.
When the catheter is in place, painful bladder contractions may occur. This may be associated with urine leakage from the catheter.
You may experience moderate burning or bleeding when urinating during the first 24 to 48 hours. Persistent bleeding may warrant prolonged use of a catheter. However, a blocked catheter caused by urinary bleeding during or after surgery (which could require a transfusion and/or a second surgery) is rare. Severe urinary tract infections are also rare.
Bladder trauma can manifest as a perforation following an obturator reflex (a sudden movement of the leg after electrical stimulation of the obturator nerve by the resectoscope). This is most common when tumours are located on the sides of the bladder, and it simply requires a catheter to be worn longer. Immediate surgical repair is very rarely needed.
Cardiovascular or anesthesia-related problems requiring an intervention and transfer to an intensive care unit are extremely rare.
How are results obtained after a bladder tumour resection?
The removed tissue is examined under a microscope by a pathologist. This medical professional performs what is called a histopathological examination.
This examination determines the presence or absence of cancerous cells in the sample. It’s also used to diagnose the type of bladder cancer. The most common is transitional cell carcinoma.
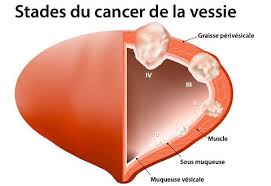
This examination will also determine how aggressive (low or high) the cancer is and whether it has spread in order to establish the stage. Most bladder tumours are superficial, but some may be invasive.
In a hospital setting, the results of the bladder tumour analysis would be reported to the attending physician after several weeks. The physician would then communicate these results to the patient in a follow-up appointment.
However, after a bladder tumour removal in a private facility through Cliniques Marois, the specimen is sent to a private pathology lab. This allows the results to be obtained much more quickly (usually within a week). A follow-up appointment with Dr. Marois is scheduled for one week after the surgery.
Once Dr. Marois has made his diagnosis, he’ll promptly propose a treatment adapted to the patient's unique situation. Some additional radiological examinations may be necessary, such as an abdominal and pelvic CT scan.
Certain intravesical treatments, such as BCG, might also be needed.
If the bladder tumor is invasive, the patient will be referred to a urologic oncology centre.


