What is a transrectal prostate biopsy?
A transrectal prostate biopsy involves sampling one or several small pieces of prostate tissue by going through the rectal wall (transrectal procedure).
Sampling is performed with the help of a special retractable needle. The doctor is guided by a transrectal ultrasound probe that makes it possible to visualize the sampling location.
A biopsy can be indicated when an anomaly has been detected by digital rectal exam, when PSA levels are high given a man’s age or when levels increase over time. This is the simplest way to sample prostate fragments without surgical intervention.
This is still the most common way to do a prostate biopsy in most hospitals or clinics.
Dr Marois does not do anymore transrectal prostate biopsy’s since the infectious complications rate is getting higher with the rise of resistance to antibiotics. He does an only transperineal prostate biopsy in all the clinic's Marois.
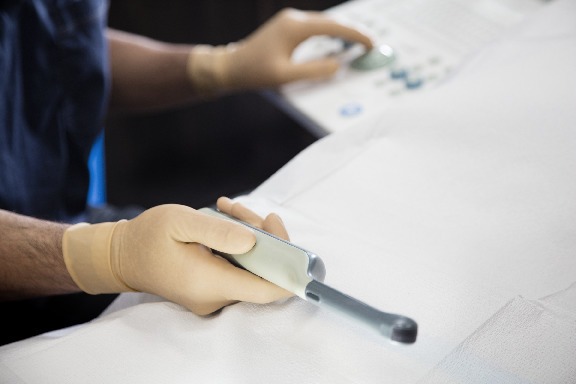
What Is the Procedure for a transrectal prostate biopsy?
First, the urologist performs an endorectal ultrasound in order to visualise the area where the sampling will be performed.
An endorectal ultrasound provides images of the prostate using an ultrasound probe introduced into the rectum via the anus.
In general, the urologist will perform a digital rectal exam before inserting the ultrasound probe, which allows him to examine the consistency of the prostate and also lubricate the area so that the introduction of the probe causes as little discomfort as possible.
The next step is to perform local anaesthesia through a transrectal route, using a small needle with Xylocaine 10cc. Patients generally report a warm, but not painful, sensation.
After this, prostate volume measurements are taken. Finally, the urologist performs the transrectal prostate biopsies. The ultrasound probe is equipped with a guidance system that allows for the visualisation of the correct entry point for the needle into the prostate and to follow its course.
The doctor uses an automatically retractable needle. This mechanism makes a “clicking” noise that can be surprising the first time. The injection itself is not painful: the needle penetrates into the prostate very quickly and retracts just as quickly.
At least 12 samples are collected from different areas of the prostate (more if the prostate is larger). When the series of samples are collected, it is best to stay seated for 15 minutes in the waiting room to avoid feelings of dizziness.
These quick and painless samples are generally well-tolerated by patients. Discomfort increases with the length of the exam and the number of samples taken. Most men report feeling only slight discomfort.
The length of the biopsy depends on the number of samples required. It usually takes about 15 minutes.
What Are the Possible Complications of Biopsy?
A course of antibiotics is prescribed before the exam to avoid infection. Prostate infection after biopsy is rising to 6 % of cases.
In case of fever appears after the biopsy (temperature over 38.5 °C), the patient must immediately go to the emergency room. It is imperative not to wait at home because this can cause a serious case of sepsis requiring intensive care if there is any delay. The emergency room doctor must be informed that you underwent a prostate biopsy under antibiotic treatment. Very specific treatment must be undertaken as quickly as possible.
Hospitalisation in the intensive care unit is possible in the case of sepsis (severe infection).
It is recommended to avoid intense physical activity for 48 hours following the exam.
How to prepare for a transrectal prostate biopsy?
Since the exam is done under local anaesthetic, the patient does not need to fast. To be more comfortable, it is recommended he urinate before the biopsy.
It is important that the patient tell the doctor what medications he is taking, in particular, any medication of the aspirin or anticoagulant type since these medications reduce the quality of blood coagulation and increase the risk of bleeding.
Recommendations after a transrectal prostate biopsy?
- The results of the samples from the prostate biopsy are communicated to the doctor after several weeks. The doctor then tells you your results.
- An appointment is scheduled for about 1 month after the biopsy.
- When the results come back “negative”, that means the samples show no cancerous abnormalities.
- Once Dr Marois has made a diagnosis of prostate cancer, he then proposes a treatment adapted to the patient’s situation.


